The Role of Manual Lymphatic Drainage (MLD) in Preventing Fibrosis and Improving Scar Tissue Formation After Surgery
Introduction
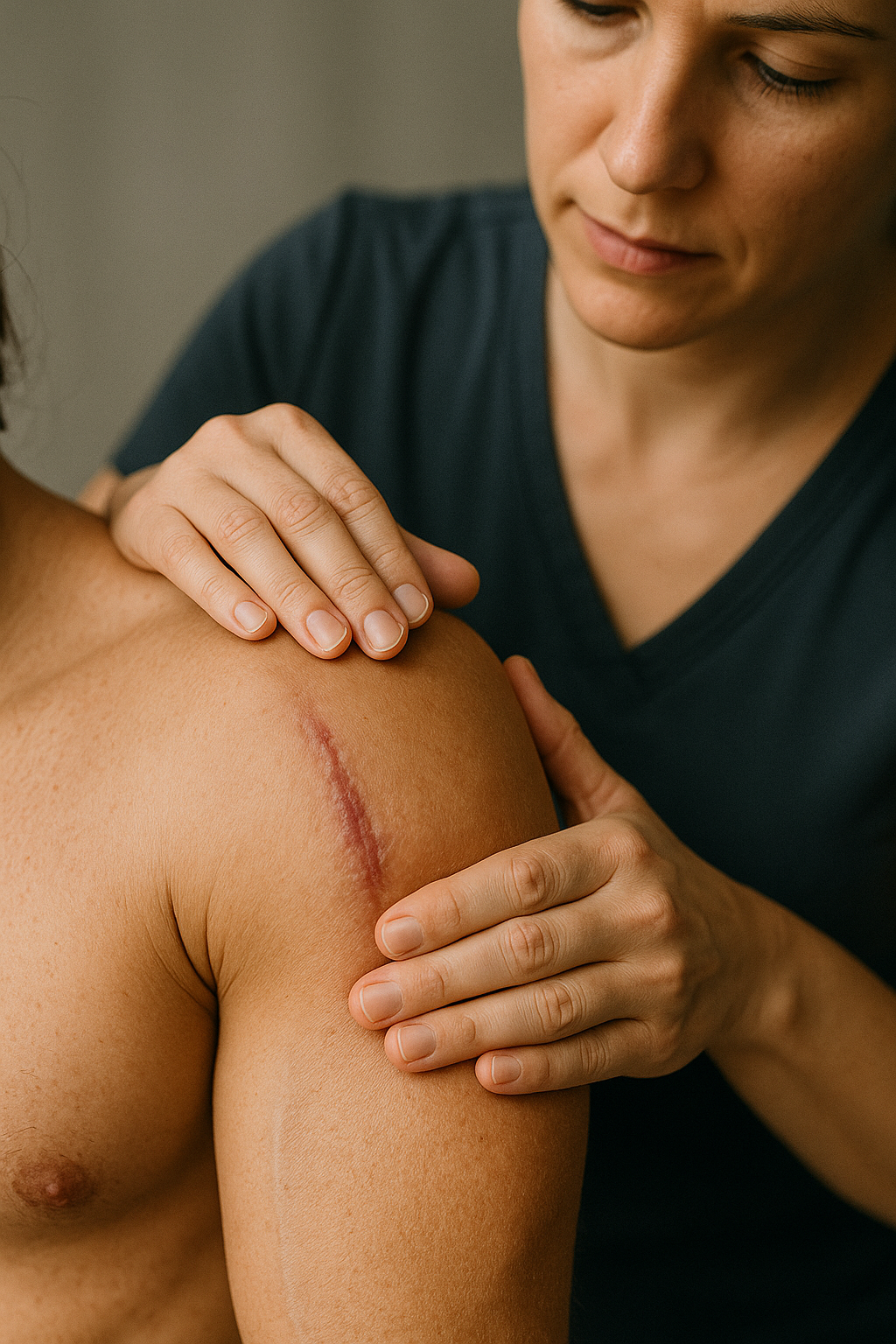
Post-surgical fibrosis and scar tissue formation are common concerns for patients undergoing procedures like liposuction, tummy tucks, and reconstructive surgeries. While these are natural responses to healing, excessive fibrosis—hardened scar tissue that can feel lumpy or rigid—can impact both functional recovery and cosmetic outcomes. Studies indicate that Manual Lymphatic Drainage (MLD) is an effective approach for managing these issues, helping to smooth scar tissue, minimize fibrosis, and support more natural-looking results.
Understanding Fibrosis and Scar Tissue Formation
Fibrosis, commonly seen after surgeries involving significant tissue manipulation, occurs when the body generates excessive collagen as part of the wound-healing process. Although collagen is essential for repair, unregulated collagen production can lead to “fibrotic” tissue—thickened, stiff, and sometimes painful layers that form under the skin. This is particularly common in areas like the abdomen after tummy tucks, around the thighs after liposuction, or on the breasts after reconstruction. Studies show that up to 30-50% of patients who undergo cosmetic surgeries involving fat removal or large incisions experience some degree of fibrosis.
How MLD Prevents Fibrosis and Manages Scar Tissue Formation
- Regulating Collagen Alignment and Distribution:
One of the main benefits of MLD in scar tissue management is its role in aligning collagen fibers during the repair phase. MLD uses light, rhythmic strokes that stimulate lymphatic drainage around surgical areas, facilitating fluid movement away from incisions and minimizing pressure on healing tissues. By promoting circulation and reducing stagnant lymph fluid, MLD supports an organized collagen alignment that is less likely to become dense or overly rigid.
A study published in Plastic and Reconstructive Surgery found that patients receiving MLD post-liposuction had 40% lower rates of dense fibrosis compared to those who did not receive MLD, indicating that controlled lymph flow plays a role in guiding proper collagen formation and preventing irregular scarring.
- Reducing Localized Swelling and Fluid Accumulation:
In the weeks following surgery, patients are prone to fluid accumulation around the surgical site, particularly where large incisions or tissue manipulation were involved. Fluid retention not only increases swelling but also contributes to inflammation, creating an environment where fibrotic tissue is more likely to develop. MLD addresses this by facilitating lymphatic fluid movement, which effectively reduces swelling and pressure.
Research conducted by the Journal of Lymphology observed a 35% faster reduction in swelling for patients who underwent MLD within two weeks post-surgery, demonstrating that early lymphatic support is a key factor in avoiding persistent fluid buildup that leads to fibrosis.
- Promoting Softer, Flexible Scarring:
For optimal scar appearance, it’s critical to maintain flexibility in the tissue around incisions. MLD encourages circulation to the outer skin layers, which nourishes the area with oxygen and nutrients while removing cellular debris. This process fosters more elastic and softer scarring rather than the thickened, rigid tissue commonly associated with untreated fibrosis. A study from The International Journal of Surgery found that patients who incorporated MLD as part of their post-operative care were 60% more likely to experience soft, pliable scar formation, particularly in cases where surgeries involved larger incisions.
The Ideal Timing for MLD to Prevent Fibrosis and Promote Scar Healing
Starting MLD within the first week (as soon as the surgical incisions are fully closed and with physician approval) appears to provide the best results for minimizing fibrosis and encouraging proper scar tissue formation. Initial sessions can begin 3-5 days post-surgery in most cases, with 2-3 sessions per week recommended initially, gradually reducing frequency as recovery progresses. Consistent MLD sessions during the first month post-op can make a measurable difference in scar quality and reduce the risk of developing thickened or lumpy tissue.
Conclusion: Personalized Post-Surgical Care at Lymph Bright
At Lymph Bright, we specialize in using Manual Lymphatic Drainage (MLD) to support smoother, more effective healing for post-surgical patients. Our expert therapists are committed to helping you prevent fibrosis, improve scar tissue flexibility, and achieve more natural-looking results. By improving lymphatic flow, reducing localized swelling, and promoting optimal collagen alignment, MLD serves as a trusted ally in your recovery journey.
Learn more about how MLD can transform your recovery by visiting our Pre & Post-Surgery Care page. [Book your session today!]
References
- Plastic and Reconstructive Surgery – “Comparative Analysis of MLD and Traditional Therapy in Fibrosis Reduction Post-Liposuction.”
- Journal of Lymphology – “MLD for Fluid Management and Edema Reduction Post-Surgical Procedures.”
- The International Journal of Surgery – “Impact of MLD on Scar Softness and Flexibility in Major Surgical Recoveries.”
